The chief executive of a prominent global nursing organization has expressed grave concern over the escalating phenomenon of high-income nations aggressively recruiting nurses from less affluent countries, labeling the situation as “out of control.”
These remarks have surfaced at a time when the BBC has uncovered compelling evidence illustrating the detrimental impact of this trend on Ghana’s healthcare system, commonly referred to as the “brain drain.”
Ghana has been grappling with a significant shortage of specialized nurses as a result of an exodus of healthcare professionals seeking higher remuneration abroad. The lure of better-paying positions in foreign lands has prompted numerous skilled nurses to abandon their posts in Ghana, exacerbating the strain on the country’s already struggling healthcare infrastructure.
Howard Catton from the International Council of Nurses (ICN) is concerned about the scale of the numbers leaving countries like Ghana.
“My sense is that the situation currently is out of control,” he told the BBC.
“We have intense recruitment taking place mainly driven by six or seven high-income countries but with recruitment from countries which are some of the weakest and most vulnerable which can ill-afford to lose their nurses.”
The extent of this issue was brought to light when it was revealed that in the year 2022 alone, over 1,200 nurses from Ghana joined the nursing register in the United Kingdom.
This sizable influx of Ghanaian nurses into the UK workforce serves as a stark illustration of the scale at which high-income countries are actively recruiting from nations grappling with limited resources and fragile healthcare systems.
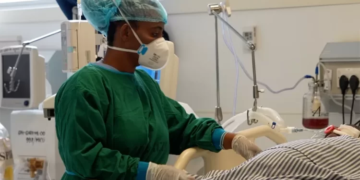
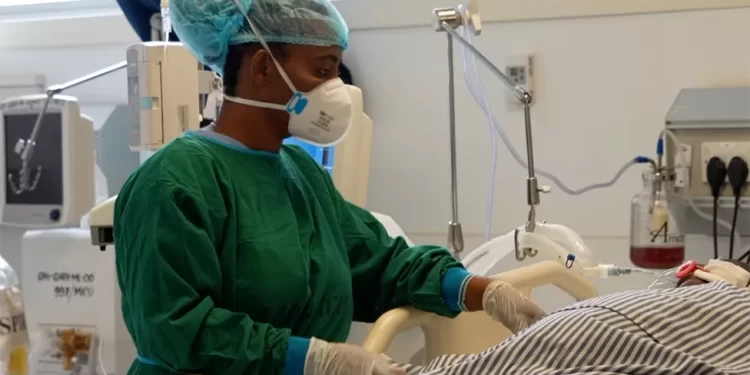
The head of nursing at Greater Accra Regional Hospital, Gifty Aryee, told the BBC her Intensive Care Unit alone had lost 20 nurses to the UK and US in the last six months – with grave implications.
“Care is affected as we are not able to take any more patients. There are delays, and it costs more in mortality – patients die,” she said.
She added that seriously ill patients often had to be held for longer in the emergency department due to the nursing shortages.
One nurse in the hospital estimated that half of those she had graduated with had left the country – and she wanted to join them.
‘All our experienced nurses gone’
The BBC found a similar situation at Cape Coast Municipal Hospital.
The hospital’s deputy head of nursing services, Caroline Agbodza, said she had seen 22 nurses leave for the UK in the last year.
“All our critical care nurses, our experienced nurses, have gone. So we end up having nothing – no experienced staff to work with. Even if the government recruits, we have to go through the pain of training nurses again.”
Smaller clinics are also affected by staff migration because even one nurse leaving a small health centre can have a large knock-on effect.
At Ewim Health Clinic in Cape Coast, one nurse has left their small emergency department and another has left the outpatient unit. Both nurses were experienced and had found jobs in the UK.
The chief doctor there, Dr Justice Arthur, said the effects were enormous.
“Let’s take services like immunisation of children. If we lose public health nurses, then the babies that have to be immunised will not get their immunisation, and we are going to have babies die,” he told the BBC.
He said adult patients would also die if there were not enough nurses to look after them after surgery.
Most of the nurses that the BBC team spoke to wanted to leave Ghana due to the fact they could earn more elsewhere.
At Kwaso healthcare centre near the city of Kumasi, Mercy Asare Afriyie explained that she was hoping to find a job in the UK soon.
“The exodus of nurses is not going to stop because of our poor conditions of service. Our salary is nothing to write home about and in two weeks you spend it. It’s from hand to mouth.”
Ghanaian nurses told the BBC that in the UK they could get more than seven times what they are receiving in Ghana.
Perpetual Ofori-Ampofo from Ghana’s Nurses and Midwives Association said her country’s healthcare system needed more help.
“If you look at the numbers, then it is not ethical for the UK to recruit from Ghana because the number of professional nurses compared to trainee or auxiliary nurses is a problem for us,” she said.
But she added that it was not possible to stop nurses from leaving as migration was a right and that the Ghanaian government needed to do more to persuade them to stay. The health ministry in the capital, Accra, declined to comment.
Fewer nurses in Ghana means that critical care for patients there is being affected, medics say
Ghana is on the World Health Organization’s list of 55 vulnerable countries, which have low numbers of nurses per head of population. The list – dubbed by some as the “red list” – is designed to discourage systematic recruitment in these countries.
The UK government recently gave £15m ($18.6m) to Ghana, Nigeria and Kenya to help boost their healthcare workforces.
But the country is known to be looking at brokering a formal deal with Ghana whereby it might be able to recruit more proactively in return for giving the government there a sum of money per nurse.
It already has a similar agreement with Nepal.
But the ICN’s Mr Catton questioned whether it was enough.
He told the BBC that he believed such deals were “trying to create a veneer of ethical respectability rather than a proper reflection of the true costs to the countries which are losing their nurses”.
The WHO’s Director of Health Workforce, Jim Campbell, explained to the BBC that Brexit had been a factor in the UK turning to African countries for nurses to fill NHS vacancies.
“The labour market is extremely competitive around the world and, having closed off the potential labour market from European freedom of movement, what we’re seeing is the consequences of that in terms of attracting people from the Commonwealth and other jurisdictions.”